In-depth analysis of dental implant risks and how to control risks in Implant treatment
When searching for information before getting dental implants, many patients ask the question: What are the risks of teeth implants? This is not only a common question, but also a very “correct” one, because any medical intervention, especially a procedure that directly involves the jawbone like Implant, carries certain risks. However, what is important to understand is that dental implant risks are not a reason to refuse Implant, but a factor that needs to be identified and controlled through expertise, technology, and a well-structured treatment system. A safe Implant case is not a case with “no risks”, but a case where risks are anticipated, controlled, and properly managed.
1. Risks in Implant placement
Dental implant risks can occur at different stages, from the time of surgery to long-term use, and each stage has its own specific groups of risks that need to be clearly understood.
1.1. Risks during surgery
This is the initial stage, and also the stage where the doctor directly intervenes in the jawbone to create the osteotomy and place the Implant into the planned position. From a professional perspective, this is the moment that determines the biological and mechanical foundation of the entire treatment case. If errors occur at this stage, the consequences do not only stop at a few postoperative days, but may affect the entire osseointegration process, prosthetic phase, and even long-term chewing function and sensation of the patient.
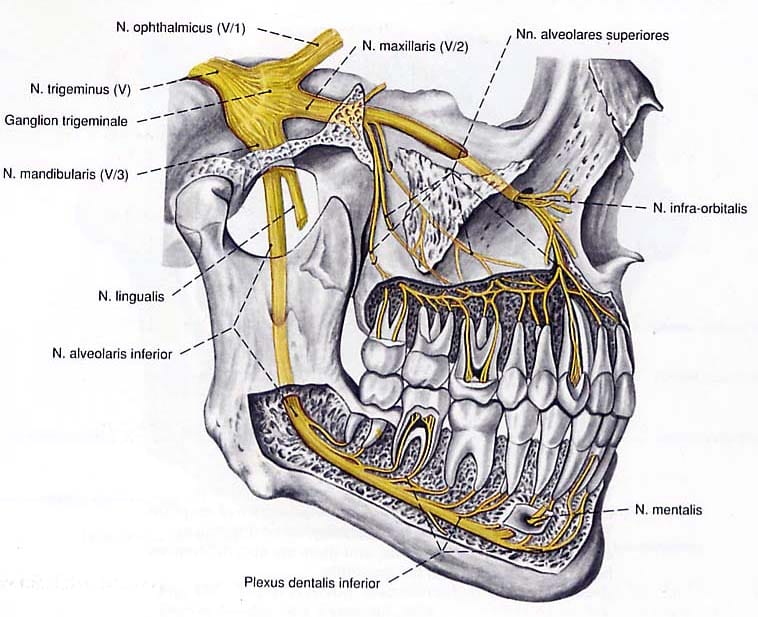

Damage to important anatomical structures
This is a serious risk and the most frequently mentioned in Implant surgery, because the jawbone is not an “empty block of bone”, but contains and is surrounded by many important anatomical structures such as nerves, blood vessels, maxillary sinus, nasal cavity, and adjacent tooth roots. If the doctor places the implant in the wrong position, direction, or depth, these structures may be damaged.
Inferior alveolar nerve injury
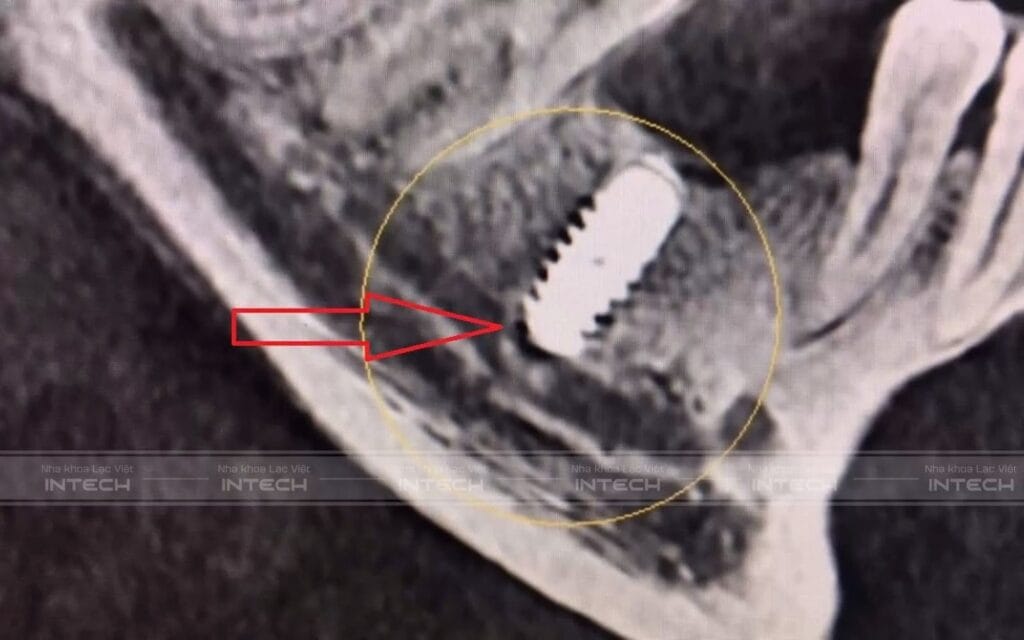
In the lower jaw, especially in the premolar and molar regions, there is an important structure within the bone called the inferior alveolar nerve canal. Inside this canal is the neurovascular bundle responsible for sensation of the lower lip, chin, and part of the cheek. If during drilling or implant placement the doctor does not accurately determine the safe distance from the nerve, the implant may contact, compress, or penetrate the canal.
The consequences of this complication can vary in severity. Mild cases may involve temporary numbness of the lip or chin for a few days or weeks. More severe cases may involve prolonged numbness, paresthesia, tingling, burning sensation, or neuropathic pain, significantly affecting daily life. In severe and late-treated cases, nerve damage may result in long-term sequelae or may be very difficult to fully recover.
It is important to note that this complication is not only due to “incorrect implant placement”, but can also result from inaccurate radiographic interpretation, incorrect distance estimation, or lack of precise placement technology. Therefore, this is a typical complication showing that Implant cannot be performed based on subjective estimation.

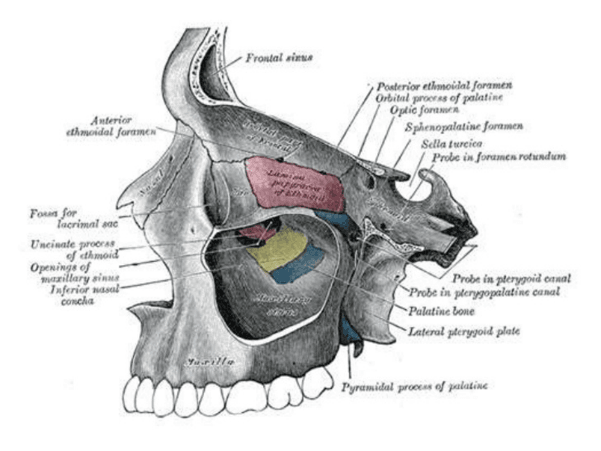
Maxillary sinus injury
In the upper jaw, especially in the molar and premolar regions, the maxillary sinus lies above the jawbone. After long-term tooth loss, the sinus tends to pneumatize downward, reducing the remaining bone height. If the doctor does not correctly assess bone height, or places the implant too deep, the implant may invade the sinus.
This complication may cause facial heaviness, sinus pain, chronic sinusitis, nasal discharge, or failure of osseointegration if infection occurs. In addition, when the implant enters or is too close to the sinus floor, prosthetic rehabilitation becomes more difficult, and sometimes the patient must undergo additional complex treatment procedures.

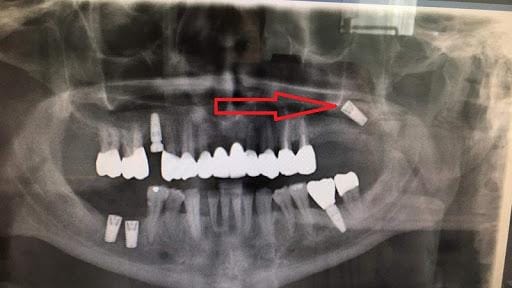

Damage to adjacent tooth roots
In cases of single tooth loss or narrow edentulous spaces, if the implant is placed too close to adjacent natural teeth, the drill or implant may damage the neighboring root. The severity can range from mild prolonged discomfort to more severe conditions such as apical inflammation, root resorption, or loss of pulp vitality.
This complication does not always appear immediately. In some cases, patients may not notice anything initially, but after a few weeks or months, the adjacent tooth may become painful, discolored, or develop apical lesions. This is a risk showing that implant placement must not only be “correct for the missing tooth position”, but also must respect and protect surrounding structures.
Bleeding during surgery
Bleeding is a surgical risk that can occur in any invasive procedure, and Implant is no exception. In most cases, bleeding is mild and can be controlled by standard measures. However, in some special cases, bleeding can become a serious issue.
The risk increases in patients with systemic conditions such as uncontrolled hypertension, coagulation disorders, liver disease, or those taking anticoagulants or antiplatelet drugs. In addition, if the drilling direction deviates and damages blood vessels in bone or soft tissue, bleeding may be greater than expected, making the surgical procedure more difficult and affecting healing.
Not only the amount of blood loss is a concern. Excessive bleeding also makes the surgical field difficult to visualize, increases the risk of procedural errors, and reduces the ability to form a stable blood clot after surgery.
Anaphylactic shock
This is a rare but very dangerous complication that can be life-threatening if not managed promptly. Anaphylactic shock may occur due to reactions to local anesthetics, antibiotics, analgesics, or certain materials used during treatment.
Symptoms may begin with urticaria, itching, difficulty breathing, hypotension, rapid heartbeat, and quickly progress to shock if not treated immediately. Although the incidence is low, this is why any facility performing Implant must have a protocol for allergy screening, emergency equipment, and a team capable of handling anaphylaxis.
1.2. Early postoperative risks
After the implant has been placed into the bone, everything is not finished. In fact, this is the stage where the body begins to “decide” whether the implant will be accepted and integrated long-term. The early postoperative phase lasts from a few days to a few weeks, sometimes the first few months, and is a very sensitive period. If problems occur during this stage, the risk of early implant failure increases significantly.
Postoperative bleeding
If intraoperative bleeding is a surgical issue, postoperative bleeding relates to healing and postoperative management. Some patients may experience prolonged oozing or even active bleeding after anesthesia wears off. This may be due to unstable blood clot formation, excessive surgical trauma, vigorous rinsing, frequent spitting, early physical activity, or underlying coagulation disorders.
Although most cases can be managed, prolonged bleeding may cause anxiety, increase infection risk, and affect initial healing.
Infection
Infection is one of the early complications that both doctors and patients must be highly cautious about. Symptoms typically include increasing pain instead of decreasing, swelling, redness, discharge, bad odor, or fever. Infection may originate from inadequate sterilization, improper postoperative care, tissue necrosis, or bacterial contamination from food and oral environment.
If detected early and mild, infection can be controlled with medication and hygiene. However, if it spreads or directly affects the bone–implant interface, it may lead to loss of osseointegration and early failure.
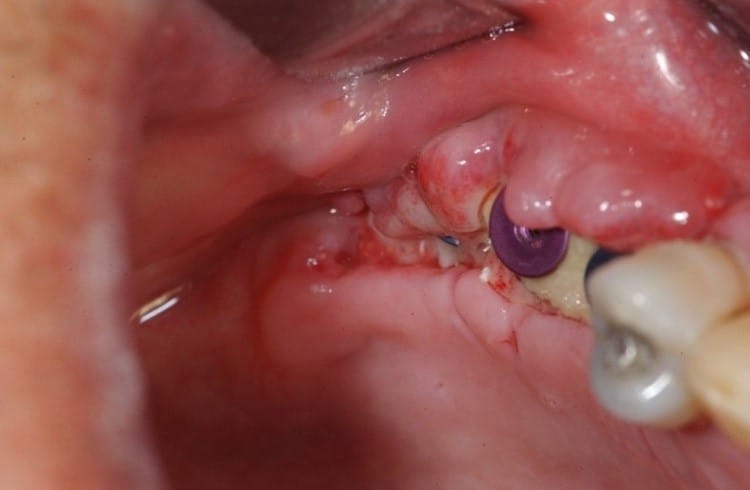

Failure of osseointegration or poor integration
This is the most critical risk in the early postoperative stage. Essentially, Implant is only successful when the jawbone forms a stable biological connection with the implant surface. This process is called osseointegration. If it does not occur or is insufficient, the implant may become mobile, painful under load, or require removal.
The causes are diverse: poor bone quality, thermal damage during drilling, insufficient primary stability, infection, smoking, uncontrolled diabetes, or premature loading before bone healing. Some cases do not completely fail but have poor integration, significantly reducing long-term prognosis.
It is important to note that failure of osseointegration is not always due to “patient factors”. In many cases, it results from improper planning, inaccurate placement, or inadequate postoperative care.
1.3. Risks after long-term use
This group of risks is often underestimated by patients. Many people assume that once the implant has healed and the crown is placed, the treatment is completely successful. In reality, an implant must not only integrate with bone but also function in the oral environment for many years under chewing forces and continuous exposure to bacteria, saliva, food, and patient habits.
Peri-implantitis
This is the most common late complication. It is an inflammatory condition of tissues around the implant, similar to periodontitis around natural teeth. Initially, patients may notice redness, bleeding, bad breath, or food impaction. If untreated, inflammation can extend to bone, causing bone loss.
As bone resorbs, implant support decreases. Patients may feel discomfort, and in severe cases, the implant may become mobile and require removal. Peri-implantitis is often related to poor hygiene, unfavorable prosthetic design, non-optimized abutment, thin soft tissue, or lack of maintenance programs.
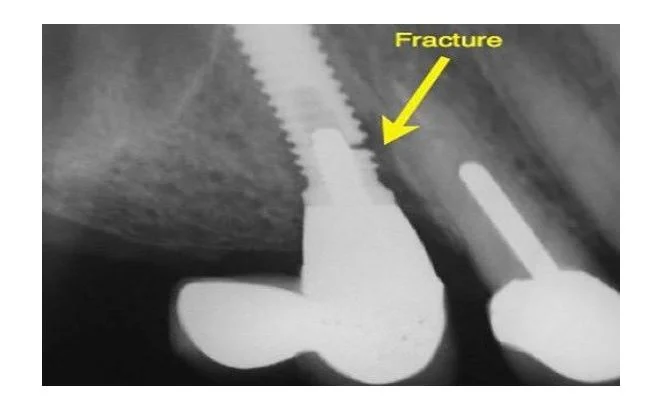
Mechanical and prosthetic complications
Implant is a system including the fixture, abutment, screw, and crown. Over time, mechanical issues may occur such as screw loosening, screw fracture, porcelain chipping, crown fracture, framework fracture in full-arch cases, or unstable chewing sensation.
These issues often arise from improper force distribution, misaligned implant placement, incorrect occlusion, poor material quality, or inappropriate prosthetic design. Some implants integrate well but require repeated prosthetic repairs due to suboptimal design from the beginning. A good implant case must be both biologically and mechanically sound.
Aesthetic and soft tissue risks
In the anterior region, aesthetics is as important as function. Over time, some patients may experience gingival recession, exposure of the implant neck, uneven gingival margins, loss of papilla, or mismatch in color with adjacent teeth.

These issues do not immediately cause implant failure but significantly affect patient satisfaction. Many cases are technically successful but aesthetically unsatisfactory. Causes often include poor soft tissue planning, lack of customized abutments, unsuitable materials, or unfavorable implant positioning.
2. Why do risks in Implant placement occur?
From an expert perspective, risks in Implant placement often revolve around 4 main groups of causes: doctor-related, technology-related, material-related, and patient-related factors. Understanding each of these factors not only helps doctors better control treatment, but also helps patients make the right choice from the beginning – the key factor to minimizing risks.
2.1 Doctor-related risks – the most decisive factor
In Implant placement, the doctor is not only the one performing the surgery, but also the one who diagnoses, plans treatment, controls risks, and determines the final outcome. Therefore, if there is any deviation from the human factor, risks are almost unavoidable.
First, risks may come from incomplete or inaccurate diagnosis. If the doctor does not thoroughly evaluate bone condition, nerve position, maxillary sinus, bone density, or soft tissue condition, the implant placement plan may be incorrect from the beginning. This leads to risks such as incorrect implant position, wrong angulation, or improper depth, resulting in consequences such as nerve damage, sinusitis, or difficulty in prosthetic restoration.
Next is the issue of suboptimal treatment planning. A good Implant plan is not simply “placing the implant into bone”, but must aim for the final outcome: good chewing function, harmonious aesthetics, proper force distribution, and long-term sustainability. If the plan focuses only on implant placement without considering prosthetics, occlusion, and load distribution, then even if osseointegration occurs, complications may still arise during use.
In addition, surgical technique is also a key factor. An inexperienced doctor may cause excessive trauma, damage bone tissue, reduce primary stability, or lead to infection. In contrast, an experienced doctor knows how to control drilling force, temperature, implant angulation, and soft tissue handling to optimize osseointegration conditions.
In summary, the doctor factor determines almost the entire “path” of the Implant case. A small deviation in diagnosis or technique can lead to major risks later.
2.2 Technology-related risks – when lacking precise control tools
In modern dentistry, Implant is no longer a field that depends entirely on “subjective manual skill”, but increasingly relies on technology to improve accuracy and reduce risks. When technology is lacking or not fully applied, the risk of error increases significantly.
First is the lack of 3D imaging diagnosis (CT Cone Beam). If only 2D images or clinical examination are used, the doctor will find it difficult to accurately assess bone height, width, density, as well as nerve and sinus positions. This increases the risk of incorrect implant placement or invasion of important anatomical structures.
Next is the lack of navigation and surgical guidance technology. Without surgical guides or navigation systems such as X-Guide, implant placement depends heavily on personal experience. Even highly skilled doctors may still have a margin of error, especially in complex cases or limited bone conditions.
In addition, the absence of minimally invasive supporting technologies such as high-frequency ultrasound, magnetic surgery, or Plasma may result in greater surgical trauma, increased swelling and pain, longer recovery time, and negatively affect osseointegration.
Technology does not replace the doctor, but it helps the doctor perform correctly and more precisely. Lack of technology means increasing unnecessary risks.
2.3 Material-related risks – the factor determining long-term durability
A common mistake among many patients is focusing only on “which implant brand”, while overlooking the fact that Implant is a system consisting of multiple components.
A complete Implant case includes:
- Implant fixture
- Abutment
- Crown
If just one of these three components is of poor quality, the entire system can be affected.
Regarding the implant fixture, if products of unclear origin or low quality are used, osseointegration ability and long-term stability will be compromised. However, even if the fixture is good, if the abutment is not suitable or not customized, it may lead to gaps, food impaction, gingival inflammation, and peri-implantitis.
The crown also plays an equally important role. If poor materials are used, improper design or incompatibility with occlusal forces, patients may experience chipping, fracture, occlusal discrepancies, or overload on the implant.
Therefore, risks do not lie in a single material, but in the consistency and quality of the entire prosthetic system.
2.4 Patient-related risks – the often underestimated factor
In addition to doctor, technology, and materials, the patient is also an important factor affecting Implant outcomes. In many cases, risks do not come from the initial treatment, but from the patient’s habits and health condition.
One of the biggest factors is smoking. Nicotine reduces blood supply, affects healing, and increases the risk of peri-implantitis. Heavy smokers have a significantly higher implant failure rate.
Next are systemic conditions such as diabetes, osteoporosis, cardiovascular disease, or immune-related conditions. If not well controlled, these conditions may reduce osseointegration ability and increase complication risks.
In addition, oral hygiene and post-treatment care awareness play a major role. Implant cannot “exist on its own” without proper care. Poor brushing, lack of flossing, and failure to attend regular check-ups may lead to peri-implantitis and bone loss.
Finally, the most important factor from the patient side is the choice of dental clinic. A wrong choice from the beginning can lead to all subsequent risks.
3. How to ensure safe Implant treatment?
The answer is very clear: the patient has only one way – to choose correctly.
Choosing correctly is not choosing the cheapest option, but choosing the right treatment system based on the following 4 core pillars:
3.1 Doctor quality – the factor determining treatment outcome
In Implant placement, the doctor is not only the one performing the technique, but also the one who diagnoses, plans, and controls the entire treatment process. Therefore, doctor quality is the most important factor determining safety and success.
A good Implant doctor must ensure three factors: professional qualification, clinical experience, and clear legal status. Professional knowledge helps the doctor deeply understand jaw anatomy, osseointegration biology, and prosthetic principles. Clinical experience helps handle complex cases, especially weak bone, long-term tooth loss, or cases requiring bone grafting and sinus lifting. Legal status ensures the doctor practices legally, is properly trained, and takes responsibility for the treatment.
More importantly, a good doctor does not only “place the implant correctly”, but must also create a comprehensive treatment plan aimed at the final outcome: good chewing function, natural aesthetics, and long-term sustainability. If the plan is not good, even correct technique may not lead to optimal results.
3.2 Dental technology – the tool for risk control
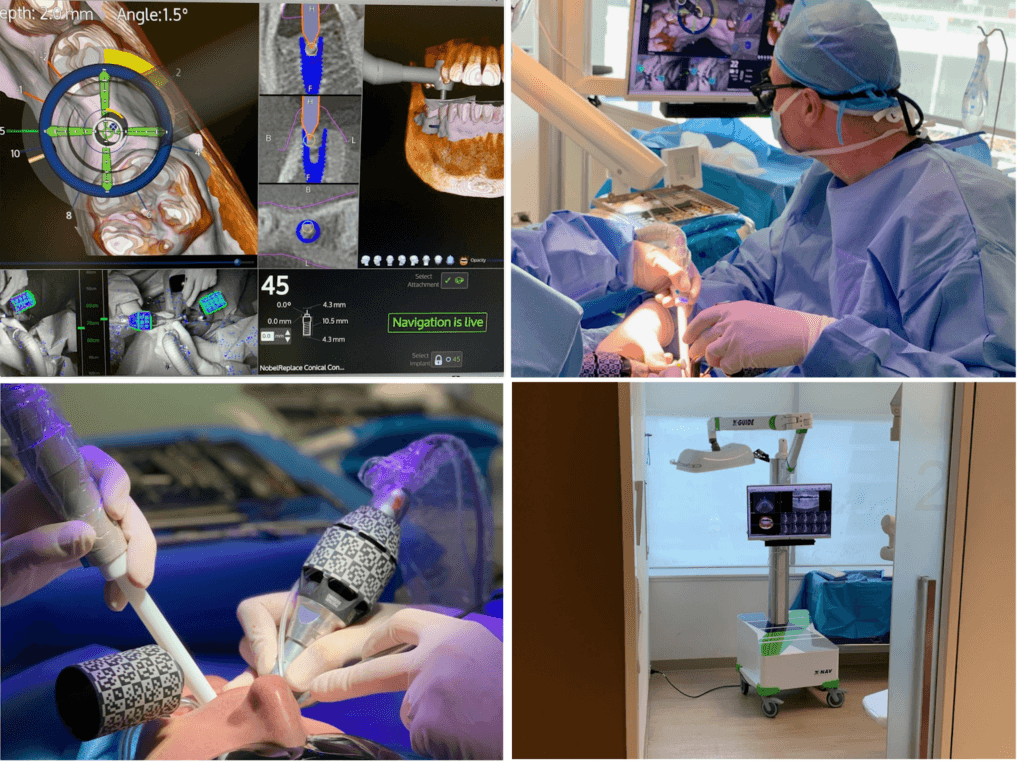
If the doctor is the “brain”, technology is the “eyes and hands” that help execute the treatment plan accurately. In Implant, technology plays a particularly important role in reducing errors and increasing safety.
First, a 3D imaging system (CT Cone Beam) is required to accurately assess bone structure, nerve position, and maxillary sinus. This is the foundation for safe treatment planning.
Next is precise implant placement technology such as surgical guides or X-Guide navigation robot. These technologies help place implants in the correct position, angulation, and depth according to the 3D plan, thereby avoiding damage to important anatomical structures and creating a foundation for accurate prosthetics.
In addition, minimally invasive technologies such as magnetic surgery, high-frequency ultrasound, and Plasma help reduce trauma, swelling, and accelerate healing. These are factors patients can directly feel after treatment.
Technology does not replace the doctor, but it helps the doctor perform correctly and more precisely. A clinic that does not invest in technology means the patient has to bear more risks.

3.3 Materials – the foundation of long-term durability
A common misunderstanding is that patients only care about “which implant brand”, while in reality, a complete Implant case is a combination of multiple components: implant fixture, abutment, and crown.
The implant fixture must be genuine, with clear origin, quality certification, and full documentation (CO, CQ). However, even if the fixture is good, if the abutment is not suitable, it may cause gaps, food impaction, and peri-implant inflammation.
Another important factor is the customized abutment, which helps shape soft tissue, improve sealing, and protect the implant neck from bacteria. This directly affects long-term peri-implant tissue health.
The crown must also be carefully selected. Multilayer zirconia is one of the optimal choices today due to its natural color reproduction, high strength, and proper force distribution, helping protect both implant and opposing teeth.
Therefore, materials are not just about “individual quality”, but about the consistency of the entire prosthetic system. A well-designed system ensures stable long-term function.
3.4 Aftercare, maintenance, and follow-up – ensuring long-term success
Implant is not a “one-time treatment”, but a long-term solution that requires monitoring and maintenance. Therefore, the clinic’s aftercare system is essential.
A reputable clinic must have a clear and transparent warranty policy, not just promises but concrete commitments regarding responsibility if problems occur. For international patients, having remote monitoring, care guidance, and support when needed is especially important.
In addition, regular follow-up visits are necessary to assess osseointegration, soft tissue condition, and occlusion, allowing early detection and timely management of problems. Regular maintenance helps extend implant lifespan and reduce future costs.
A good Implant system is not only one where “the implant is successfully placed”, but one that is maintained and functions stably throughout its lifespan.
4. Why should you choose Implant treatment at Lac Viet Intech?
When it comes to dental implant risks, the important thing is not to avoid risks, but to control them systematically. This is the treatment philosophy at Lac Viet Intech.
Lac Viet Intech has a team of specialized Implant doctors, with a treatment approach based on planning and risk control from the beginning, rather than dealing with complications afterward. The technology system is comprehensively invested, including CBCT imaging, digital scanning, surgical guides, and X-Guide navigation robot, helping increase placement accuracy and minimize the risk of anatomical damage.
>>> See more: Advanced Dental Implant Technologies at Lạc Việt Intech
In addition, Lac Viet Intech applies minimally invasive technologies such as magnetic surgery, high-frequency ultrasound, and Plasma to reduce trauma and improve healing. In terms of materials, the system uses genuine implant fixtures, customized abutments, and multilayer zirconia crowns, ensuring long-term stability and aesthetics.
An important difference is transparent pricing policy and long-term warranty commitment, helping patients, especially international patients, feel secure about post-treatment responsibility.
5. Q&A – Frequently asked questions
Is dental implant dangerous?
Not dangerous if treated correctly. The danger comes from choosing the wrong clinic.
Is the implant failure rate high?
Low if performed with proper technique and treatment planning.
Is implant painful?
There is mild discomfort, but it is fully controlled with modern technology.
How long until the implant is stable?
Typically from 2–6 months depending on bone condition and individual factors.
How to reduce dental implant risks?
Choose the right clinic, the right doctor, and the right technology.
>>> See more: Best Dental Implant Clinic Vietnam: Why Many International Patients Choose Lac Viet Intech for Dental Implant Treatment
Conclusion
What are the risks of teeth implants?
The answer is: there are risks, but they are completely controllable.
Implant is not the problem.
Wrong choice is the problem.
If you understand dental implant risks correctly and choose right from the beginning, Implant will become a safe, sustainable, and effective long-term tooth restoration solution.
Related reading for international patients
If you are comparing treatment options, you may also find these guides helpful: 5 Risks of Choosing Vietnam for Dental Implants – What International Patients Should Know Before Deciding, 5 Important Criteria to Ensure Safe and Sustainable Dental Implant Placement and Dental Implant Vietnam: The Complete Guide for International Patients Seeking Safe and Long-Lasting Treatment.
Frequently asked questions
The most common dental implant risks include infection, failed osseointegration, nerve-related complications, sinus issues in upper-jaw cases, and mechanical problems if treatment planning is incomplete.
Yes. Dental implant risks can be reduced with a detailed examination, 3D imaging, full medical history review, and treatment performed by an experienced implant specialist using modern technology.
International patients need careful risk assessment to choose the right clinic, plan their travel time and budget accurately, and reduce the risk of complications or unexpected retreatment after returning home.

Pingback: Dental Implant Cost in Vietnam 2026 - Lac Viet Intech Dental Center
Pingback: 5 Risks of Choosing Vietnam for Dental Implants and How to Avoid Them