Dental implants are currently considered the best solution for replacing missing teeth, as they can replace both the root and the crown, providing strong chewing function, natural aesthetics, and long-term durability. However, like any medical intervention, implant placement is not completely risk-free. If treatment is indicated incorrectly, diagnosis is not thorough, surgery lacks precision, or post-treatment care is inadequate, patients may face serious complications.
Among these risks, there are 3 complications that patients need to clearly understand before treatment: Implant infection, Implant nerve damage, Maxillary sinus damage. These are all complications that can directly affect treatment outcomes, oral health, and even the patient’s long-term quality of life.
The article below will help you clearly understand what each complication is, why it occurs, how to recognize the signs, and most importantly, how to prevent it.

Implant infection – What is peri-implant infection?
Implant infection is a condition in which bacteria invade the tissues surrounding the implant, causing inflammation in the gum tissue, soft tissue, and in severe cases, spreading to the bone that supports the implant. In simple terms, this is a “bacterial infection” around the implant, similar to an infected wound, but more dangerous because it occurs exactly at the area where the implant needs to integrate tightly with the jawbone.
To better understand, when an implant is placed into the jawbone, the body needs time for the bone to attach firmly to the implant surface. This process is called osseointegration. If during this period or afterward bacteria invade the surrounding tissues, an inflammatory response will occur. Initially, the inflammation may be limited to the gum, but if it persists, bacteria will destroy the bone around the implant, causing loss of support and eventual failure.
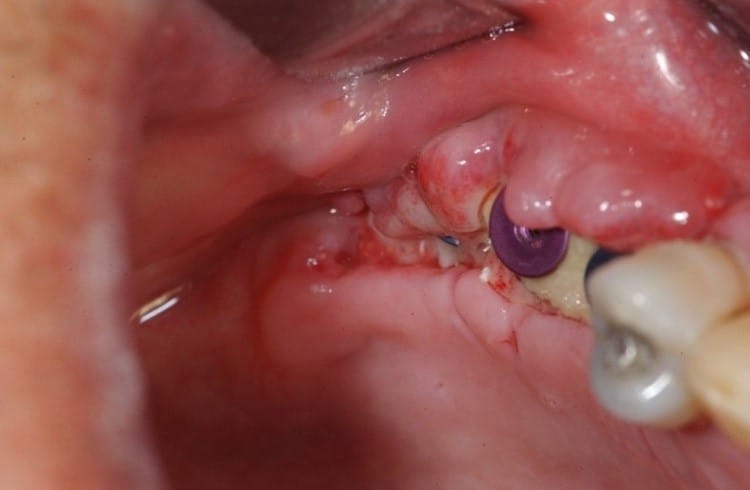
Signs of Implant infection
Patients may experience the following symptoms:
- Swelling, redness, pain, or dull aching around the implant site
- A feeling of pressure or discomfort when chewing
- Discharge or pus around the implant
- Persistent bad breath
- Bleeding around the implant when touched
- In more severe cases, the implant may feel loose or chewing becomes unstable
Why does Implant infection occur?
The causes of implant infection often result from multiple combined factors. First is poor infection control during surgery. If the surgical environment, instruments, or sterilization protocols are inadequate, the risk of bacterial contamination increases significantly. Second is improper post-operative care by the patient, poor oral hygiene, or failure to attend follow-up visits. Third is poor treatment planning and prosthetic technique, creating gaps, plaque-retentive areas, or food impaction, leading to prolonged bacterial accumulation. In addition, patients with underlying conditions such as uncontrolled diabetes, periodontitis, or heavy smoking have a higher risk of infection.
Consequences of Implant infection
If not detected early, implant infection can lead to peri-implantitis, bone loss around the implant, loss of osseointegration, and eventually implant removal. Notably, when an implant is lost due to infection, the bone in that area is often more deficient, making future re-treatment more difficult, more expensive, and more complex.
How to prevent Implant infection
To prevent this complication, patients should choose a dental clinic with a well-controlled sterilization system, experienced implant specialists, and a clear treatment plan. After treatment, patients must strictly follow medication instructions, maintain proper oral hygiene, follow dietary recommendations, and attend regular follow-ups. In the long term, plaque control around the implant is extremely important, because although implants do not decay like natural teeth, they are highly susceptible to inflammation if not properly maintained.
Implant nerve damage – What is nerve injury in dental implant placement?
Implant nerve damage is a condition where the implant or the drilling process injures, compresses, or invades a nerve. In implant dentistry, the most commonly involved nerve is the inferior alveolar nerve – a very important structure located within the lower jawbone, responsible for sensation in the lips, chin, and part of the oral region.
Simply put, you can imagine that inside the lower jawbone there is a small “canal” running along its length, containing the nerve. If the implant is placed too deep, drilled in the wrong position, or an inappropriate implant is selected, it may touch or compress this nerve. In such cases, the patient not only experiences pain but may also suffer from prolonged sensory disturbances.
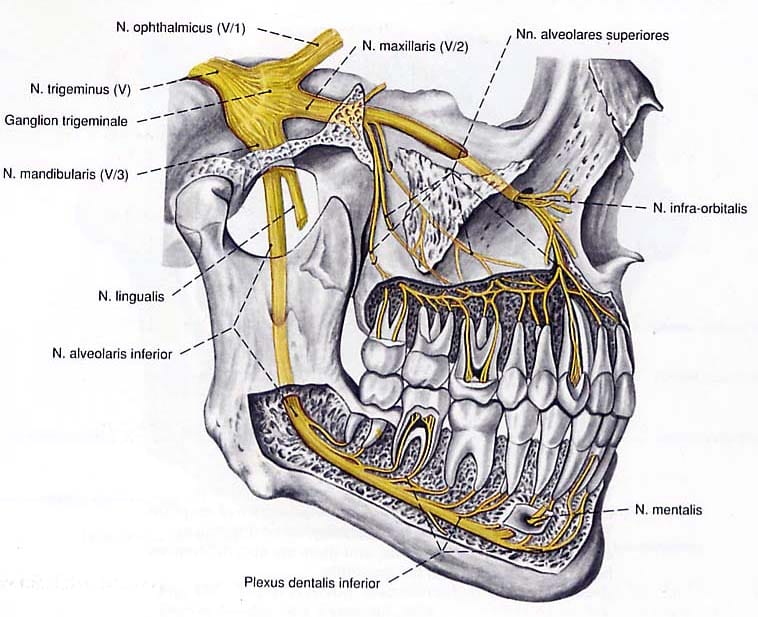
Signs of Implant nerve damage
Common symptoms include:
- Numbness of the lips or chin that does not return to normal after anesthesia wears off
- Tingling, crawling sensations, or burning in the lips or chin
- Heaviness or partial loss of sensation in part of the face
- Discomfort when eating, speaking, or touching the affected area
- In severe cases, neuropathic pain or prolonged sensory disturbances lasting months
Why does Implant nerve damage occur?
The most important cause is inaccurate diagnosis and treatment planning. If the dentist does not take a 3D Cone Beam CT scan, or takes one but does not carefully analyze the position of the nerve canal, the implant may be placed in a dangerous area. In addition, poor surgical technique, excessive insertion force, over-drilling, or using an implant that is too long are also common causes.
In other words, this complication is closely related to the accuracy of the treatment plan and surgical skill. In many cases, even a deviation of a few millimeters can lead to serious consequences.
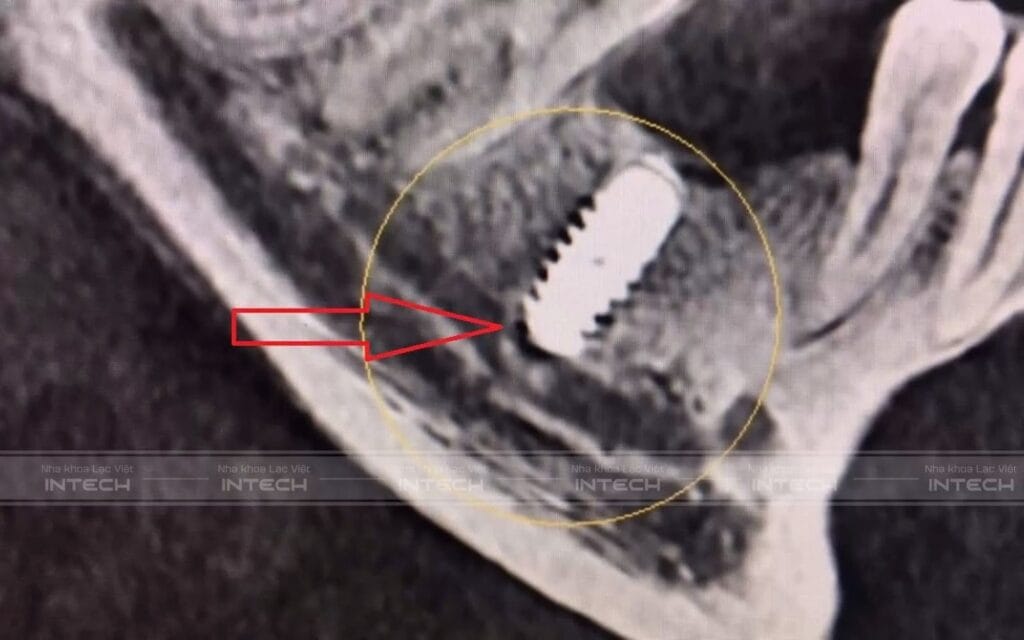
Consequences of Implant nerve damage
The consequences can range from mild to severe depending on the extent of injury. Some patients experience temporary numbness that gradually recovers. However, in more severe cases, prolonged sensory disturbances, neuropathic pain, daily discomfort, and a significant impact on quality of life may occur. More concerning is that if nerve damage persists for too long without timely intervention, the likelihood of full recovery decreases.
How to prevent Implant nerve damage
To prevent this complication, a Cone Beam CT scan must be performed to accurately evaluate jaw anatomy. The dentist should then plan implant placement in 3D space, selecting the correct implant length, diameter, and angulation. Technologies such as surgical guides or navigation systems can significantly reduce errors in high-risk areas. From the patient’s perspective, if numbness persists abnormally after implant placement, they should return immediately for evaluation rather than waiting too long.

Maxillary sinus damage – What is sinus injury in implant placement?
Maxillary sinus damage is a condition where the implant or surgical process invades the maxillary sinus. The maxillary sinus is a hollow cavity located within the upper jawbone, above the molar and premolar regions. When teeth are missing for a long time, the upper jawbone tends to resorb, while the sinus tends to expand downward. This reduces the available bone height for implant placement, increasing the risk of the implant contacting or penetrating the sinus.
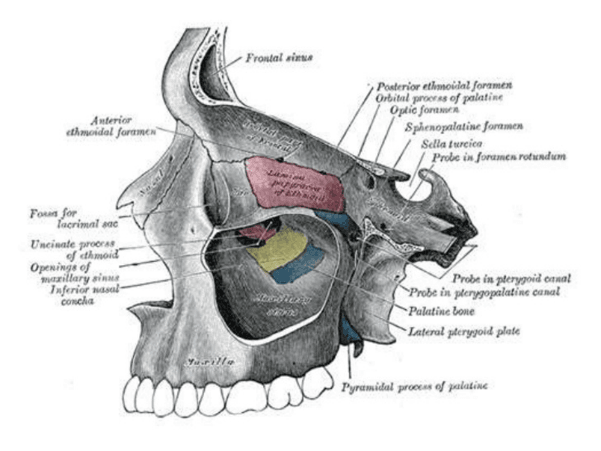
To visualize this, in the upper molar region, above the tooth roots is not a thick solid bone block, but a hollow space called the sinus. If the remaining bone height is insufficient and the implant is placed incorrectly, it may extend into this cavity.
Signs of Maxillary sinus damage
Symptoms may include:
- Dull pain in the cheek, sinus area, or headaches after surgery
- A feeling of heaviness or pressure in the upper jaw
- Nasal congestion or sinus discomfort
- Nasal discharge or sinusitis after implantation
- Persistent discomfort when bending over or changing posture
In some mild cases, symptoms may not be obvious initially. However, if the condition persists, chronic sinusitis may develop, making treatment much more complicated.
Why does Maxillary sinus damage occur?
The main cause is inadequate evaluation of the remaining bone height in the upper jaw. If the dentist does not perform 3D imaging or fails to carefully analyze the relationship between bone and sinus, selecting an implant that is too long or placing it at the wrong angle can easily lead to sinus damage. In addition, cases that require sinus lifting but are not properly indicated or performed incorrectly also increase the risk.
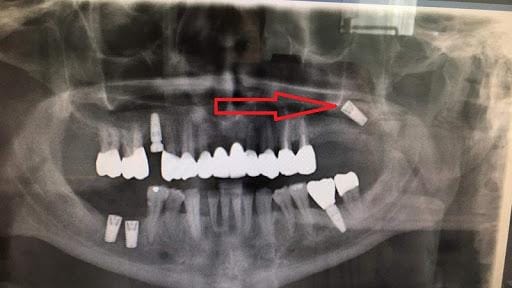
Consequences of Maxillary sinus damage
Common consequences include sinusitis, prolonged pain, facial discomfort, and the need for corrective surgery. In severe cases, the implant may need to be removed, the sinus stabilized, and only then can re-implantation be considered. This means a significantly longer treatment time, higher cost, and psychological impact on the patient.
How to prevent Maxillary sinus damage
To prevent this complication, it is essential to accurately evaluate bone volume and height in the upper jaw using Cone Beam CT. If the bone is insufficient, appropriate procedures such as sinus lifting or alternative solutions must be indicated. In addition, implant placement must be precise, with correct implant size and angulation. This complication clearly demonstrates that although implant treatment may seem similar, safety depends heavily on treatment planning and the technology used.
Why do these complications occur?
At their core, the three serious complications – Implant infection, Implant nerve damage, and Maxillary sinus damage – do not occur randomly. Most of them originate from four main groups of causes.
First is the dentist factor. Lack of experience, incorrect planning, poor prognosis, or imprecise surgery significantly increases the risk of complications.
Second is the technology factor. Implant treatment requires high precision. Without Cone Beam CT imaging, 3D planning software, surgical guides, or navigation systems, many procedures rely heavily on subjective experience, increasing the margin of error.
Third is the material and treatment system factor. Low-quality materials, incompatible components, or poor prosthetic design can increase the risk of infection, instability, and long-term complications.
Fourth is the patient factor. Patients with unstable systemic health, poor oral hygiene, heavy smoking habits, irregular follow-ups, or non-compliance with post-operative instructions are at higher risk.
In other words, implants themselves are not “dangerous”; the risk lies in whether the treatment is performed correctly.
>>> See more: Advanced Dental Implant Technologies at Lạc Việt Intech
How to make dental implant treatment safer?
From a patient’s perspective, the simplest way to reduce risk is to choose the right clinic from the beginning. A safe implant clinic must have experienced implant specialists capable of diagnosis, planning, and complication management. At the same time, it must be equipped with precise diagnostic and surgical technology, authentic materials, proper sterilization protocols, and a long-term follow-up system.
In addition, patients need to understand that implant treatment is not a “place it and forget it” procedure. Follow-up visits, hygiene maintenance, occlusal control, and periodic monitoring are all essential parts of ensuring long-term implant stability.
Conclusion
Complications such as Implant infection, Implant nerve damage, and Maxillary sinus damage are serious risks that patients need to understand before undergoing implant treatment. However, the important point is that most of these complications can be prevented if treatment is performed correctly, with proper indication and technique.
Understanding complications is not to fear implants, but to make more informed treatment decisions. A successful implant case is not just about placing the implant into the bone, but achieving safety, stability, functional chewing, aesthetics, and long-term durability.
FAQ About Dental Implant Complications
What are the 3 serious complications of dental implants?
The three serious complications explained in this article are implant infection, nerve injury, and maxillary sinus damage.
Can dental implant complications be prevented?
Most serious complications can be reduced significantly with proper diagnosis, CBCT-based planning, precise surgical technique, and careful post-operative follow-up.
Is implant infection always a sign of implant failure?
Not always. Early inflammation can often be managed if it is detected and treated promptly before major bone loss occurs.
Why is sinus or nerve damage considered a serious implant complication?
These complications can affect sensation, comfort, healing, and long-term implant stability, so they require careful prevention during treatment planning and surgery.
